This is an excellent opportunity for anyone trying to conceive. Please reach out to Dr Matthew Payne directly if you would like more information.
COVID-19 Relevant Health Guidelines
The Department of Health Western Australia has published some guidelines in relation to COVID-19. Those that are relevant to our families include ‘Management of COVID-19 Infection in Pregnant Women Statewide’ and also ‘COVID-19 Guidance for Neonatal Services Statewide’.
Whilst we hope that all those who are pregnant remain well. Given the present situation it may pay to familiarise yourselves with these documents and discuss with your care team if you have any questions.
It is important to remember to only obtain information from trustworthy sources.
"I thought I was living a nightmare."
Blog post by Mum and Volunteer Sheree.
It was a Sunday afternoon and I was relaxing watching Netflix, as I'd been feeling a bit off with a mild headache. I was 33 weeks pregnant. I remember laying there thinking surely I can't get much bigger than I currently am, and just thought I was tired from working and that was the reason for my headache.
I had a rough nights sleep that night and called in sick the next morning as I just didn't feel like I had the energy to go. I had an appointment with my obstetrician that afternoon, but I still just thought what I was experiencing was normal pregnancy symptoms. It was at that appointment I was told I was being admitted to hospital for observation as I was showing early signs of pre-eclampsia. I was scared and severely emotional.
My baby was the result of a hard journey through IVF and the very thought of any threat in my pregnancy resulting in anything other than our dram come true, was too much to bare. I was a total mess. My night that night in the hospital was full of hourly checks and observations and by morning I was told by my obstetrician than I wasn't to return to work, as I was still borderline pre-eclampsia, but I was fine to head home on bed rest.
I spent the next 4 days sitting on the couch taking it easy, but on Friday night I began to feel off - a little nauseous and that headache was back. I didn’t know whether to think too much into it or whether to go to the hospital. After an hour wondering I decided to at least call the hospital. After telling them how I was feeling they advised me to come in. So off we went to the hospital and I was hooked up to a machine to see how the baby was going. He was doing well, but I was not. The doctor told my husband and I that my liver and kidneys were showing signs of being in distress and whilst it wasn’t an absolute emergency that night, I was to stay in hospital. I thought I was living a nightmare. I was so scared for my baby and the thought of him being born early was too much for me to cope with. I was an emotional wreck.
The next three days were a routine of hourly checks and lots of blood tests. By Monday morning my obstetrician wasn’t willing to hold off any longer and I was to have a caesarean that morning, as my condition had worsened. Again with the freaking out.
The nurses were so supportive. I was taken down to the Neonatal Unit to see where my baby would go when he was born. It was weirdly comforting and intense all at the same time. The nurses talked me through what some of the machines were and what role they would play for my baby.
My son was born 3 hours later at 33 weeks and 4 days. He came out crying and weed everywhere, so I was able to hold him before he was taken away. It was this moment I hadn’t wanted to miss out, of all the moments you get when having a baby. I was so amazingly happy and so in love.
We spent 3 weeks in NICU before my son was able to come home. The nurses and doctors in our nursery were absolutely amazing. I was allowed to be my sons mother. Even though changing a baby with cords is difficult, it was amazing. The day we were told we could take him home, I panicked. We were in this safe little bubble in the nursery and it just seemed so scary that suddenly I really would be totally in charge.
My son is now 14 months old. He’s endured two surgeries in his short life, but he is healthy, happy and totally adorable. When we think back to our time in the nursery, we just remember how lucky we were that all our little man had to do was grow a little. For some this isn’t the case. The experience has made us more aware of what others sometimes have to go through, and how lucky we are. Every day with our son is amazing.
We welcome you to share your story with us. Please e-mail your story along with a few pictures to admin@tinysparkswa.org.au with 'Family Story' in the subject.
Social Impact
Late in 2017 we had the pleasure of working with some fabulous students from Curtin University on their project 'Just Causes'. They were seeking out organisations who have made significant social impact for all manner of reasons. We were honoured to be approached and can finally share their work with you. We think it's awesome, but we might be a bit biased, see for yourself.
My Strong Boy
Guest blog post by Sarah.
I was so thrilled to hear about the research recently announced by the Victor Chang Institute that vitamin B supplementation could prevent some miscarriages and birth defects.
After having my first baby with born with an abdominal wall birth defect, Gastroschisis, then suffering multiple miscarriages and having my next baby born with intrauterine growth restriction and placental insufficiency, I was relieved when my wonderful Obstetrician indicated that I could prevent my third baby suffering such things by taking vitamin B (and aspirin).
After spending many years myself working at paediatric and obstetric research institutes, although in a non-research role, I was always interested in why my pregnancies had been so troublesome and how I could've prevented them being so.
Almost ten years on, it seems fitting to share the birth story of my first born at the same time as such a momentous research announcement that could prevent many other women and babies following my same journey.
My journey with a high-risk pregnancy began at the 12-week mark of my pregnancy in 2007.
My story ends well. My high-risk baby is now a healthy, happy nine-year-old boy, an avid Dockers fan, footy mad and full of energy.
I do know, however, that other’s stories do not end like mine and that I am truly one of the lucky ones.
It was a winters day in Perth as I took myself off to my first trimester scan. Excited and nervous to see my baby, all seemed normal at my ultrasound. The Sonographer was clearly very good at keeping mum.
"Shall I post your scans to your Dr?" the Receptionist asked. "No, no - I'll take them myself" I said, hoping to have a sneaky look on my way.
Omphalocele - the letter said. What was that? This was in my pre-smart phone days, so I had to wait until I arrived at work to google it. Dr google. Worst invention ever.
"Omphalocele is an abdominal wall defect where organs protrude outside the body. Commonly associated with a high mortality and other defects".
Heart sinks.
And I'd already told everyone at work. Thankfully, I worked in a health organisation with a bunch of very understanding people.
I got straight into my Dr who referred me to King Edward Memorial Hospital (KEMH). It was a nervous week waiting for that appointment.
Immediately at ease in the care of the KEMH staff, the Sonographer confirmed that my baby had Gastroschisis. Still an abdominal wall birth defect, but with far better outcomes than Omphalocele. My baby could survive. Relief!
I was referred to the high-risk pregnancy management team at KEMH, who I could not speak more highly of, and, whilst they couldn’t guarantee me everything would be ok, they did provide me with reassurance that they would do everything they possibly could to help my baby survive.
I had many, many scans. I was told my baby had a higher risk of being born prematurely or stillborn. But – I prayed that he would enter the world alive, and for some reason, I had absolute faith that he would.
I visited the Neonatal Unit at Princess Margaret Hospital (PMH) where my baby would be transferred for surgery following his birth. He was to be in very safe hands.
Unexpectedly, I was informed that I could deliver my baby naturally, despite his exposed abdomen. And so, at 34 weeks pregnant, while sitting in my final antenatal class, I began to feel a bit strange. I headed home, put on a movie (not sure why I chose to watch Jersey Girl that night – but not a good choice if you are about to give birth!!), and waited until my contractions got closer together.
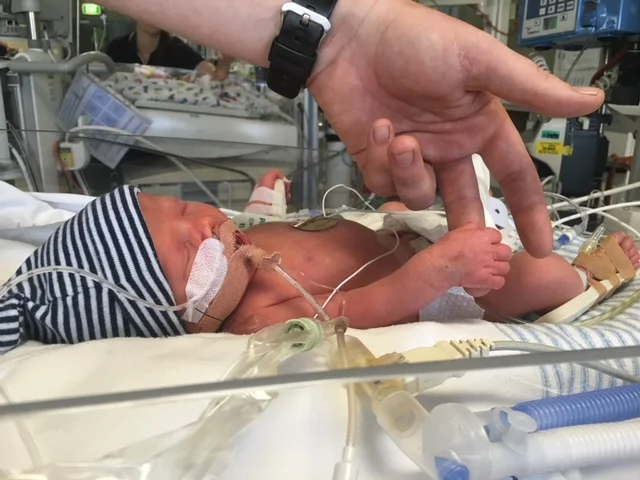
Arriving at the hospital at 1am, it was a smooth birth and my son was delivered to a room full of doctors at 9am weighing just under 2kg, on my Grandmother’s birthday.
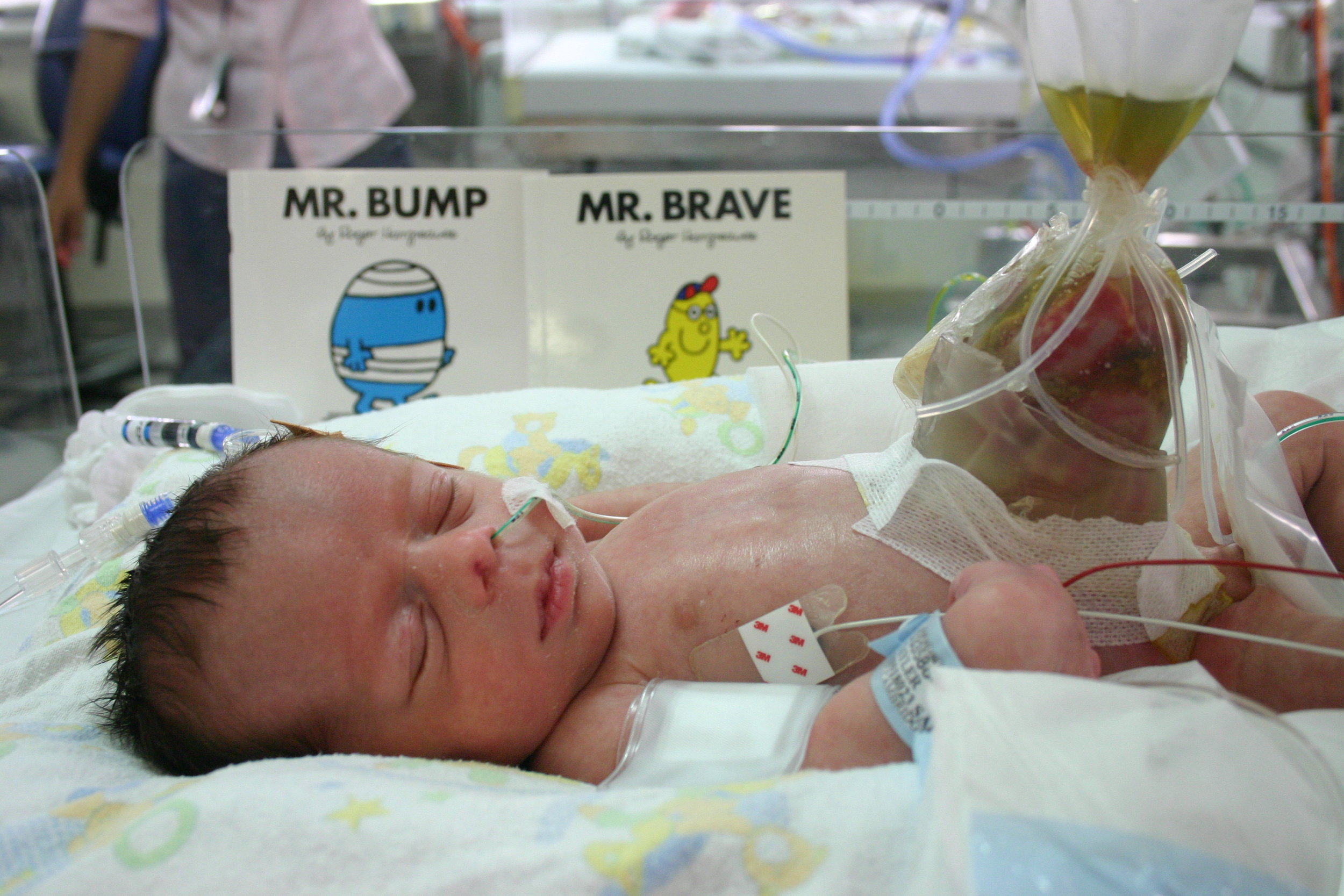
My baby, and his internal organs which covered his tiny body, was wrapped in a protective bag and I had a little hold before he was whisked away to the Neonatal Intensive Care Unit.
There only for a short while, he was transferred that same day via the Newborn Emergency Transport Service to the PMH Neonatal Unit - 6B.
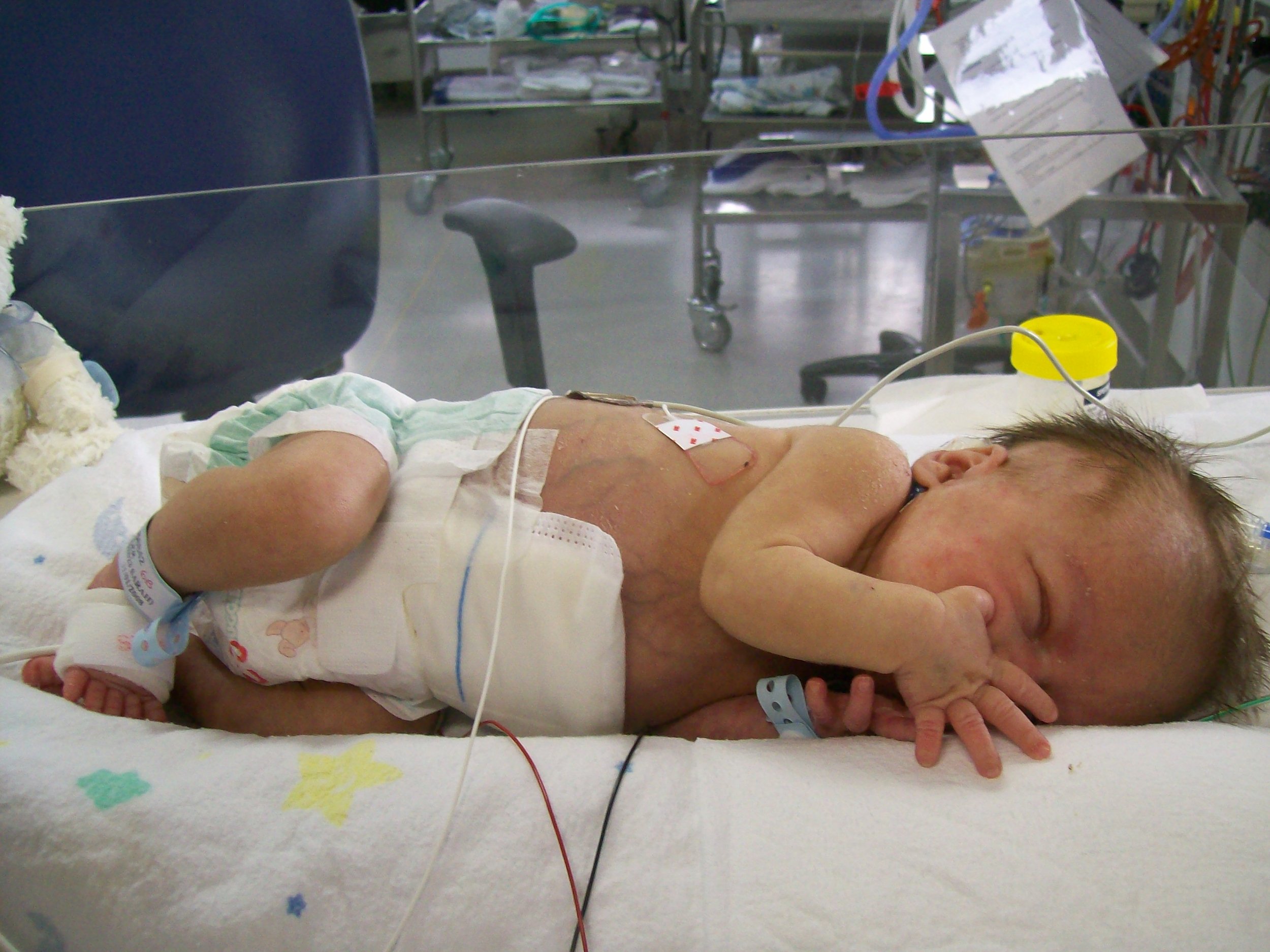
We spent 3 months in total in that unit. 3 months of tube feeding, of constant IV lines (I'll never forget the one in his head when they had run out of other veins), of 6 gruelling surgeries, and of not taking my tiny baby home with me.
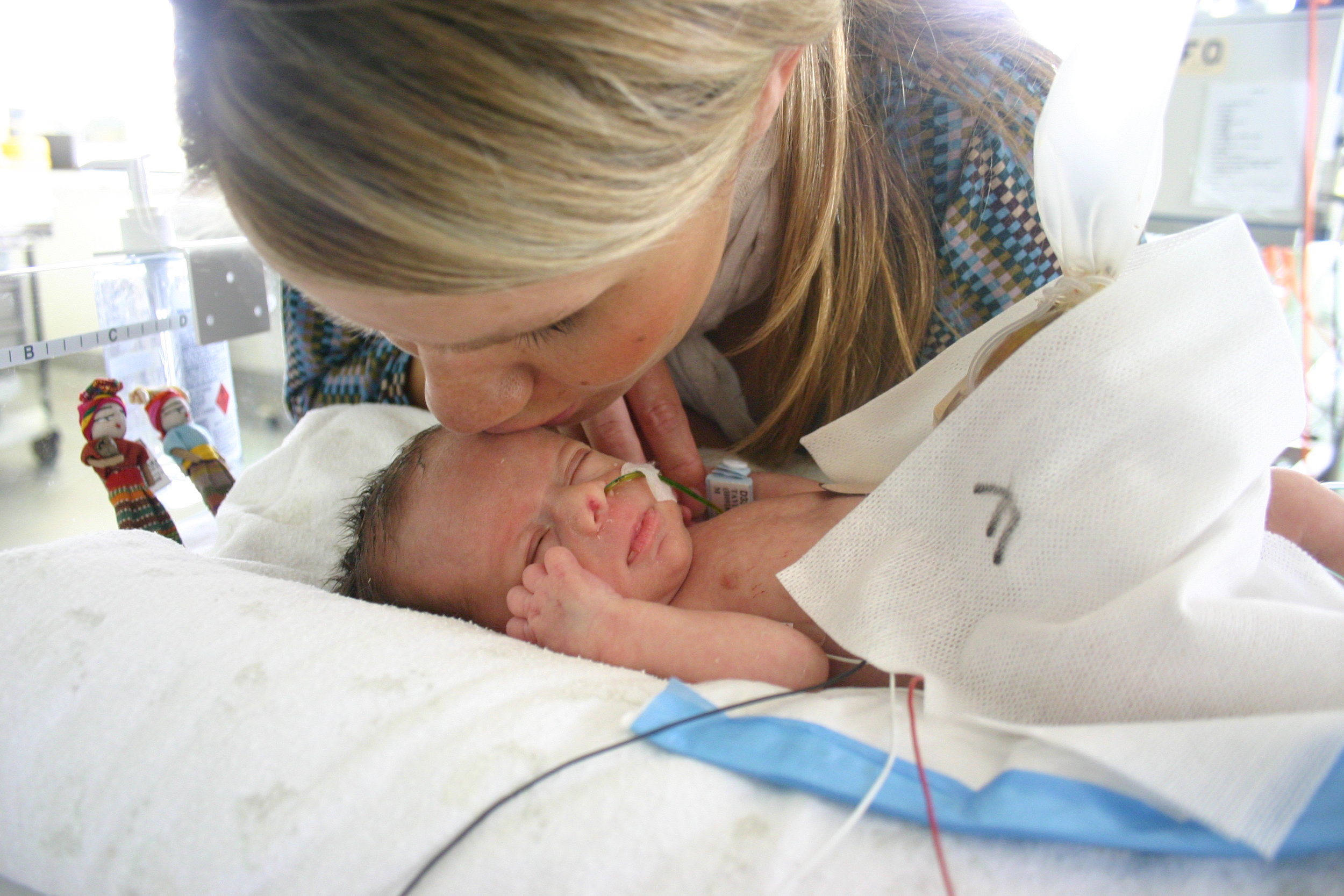
I wasn't able to hold him for 2 months, and his only comfort was the touch of my hand and a dummy that was almost as big as his tiny face. He loved that dummy!
Initially, the Surgeon tried to insert his intestines back into his body, but as they didn't develop inside him, his tummy was not large enough to accommodate them. He developed compartment syndrome, and had to be opened up again. Slowly over about a month, his intestines were held in a plastic silo that fed them back into his tummy and stretched it at the same time. It was a very long month and I distinctly remember one of the Paediatrician's updates, "he's not out of the woods yet".
I visited my baby every day. I prayed that me being there and doing everything I could would somehow help him pull through. I also expressed milk every 3 hours for those 3 months so that I could one day feed him. The milk bank was FULL of my milk!
Despite the challenges, I felt extremely lucky that he was in the care of such competent and caring medical professionals and kept thinking how fortunate it was that he was born in a generation and country where he could be helped.
Finally, after about 2 months his intestines fit inside his body. He had quite a large 'crater' in his tummy, however, from a lack of skin covering his enlarged abdomen and this took some time to heal.
But, shortly after this, I was able to hold him in my arms!
Our next challenge was getting his intestines working. There were several kinks and blockages that had developed, and this followed with more surgeries to clear them up. Short gut syndrome was a real possibility, which would have meant a lifelong problem with feeding. But, thankfully, this didn't eventuate.
His gut started to work. He could take small tube feeds, which progressed to larger feeds, and then breast feeds - finally I was able to feed him!
And then - at last - I was able to walk him outside for the first time, 3 months after he was born. We went to the local park and I felt like the luckiest person alive.
Once we were home, he did struggle to gain weight and was readmitted to hospital once, but this was the only main hiccup following his discharge.
To this day, you would not know that my normal, happy, primary school boy had such a dramatic entrance to the world unless you looked at the scar on his abdomen, and noticed the lack of his belly button.
People say that it must've been really challenging to get through his time in hospital. It certainly wasn't ideal, but being my first baby I didn't have a comparison, and I just felt very fortunate that he was cared for so well, and that my strong boy was able to live.