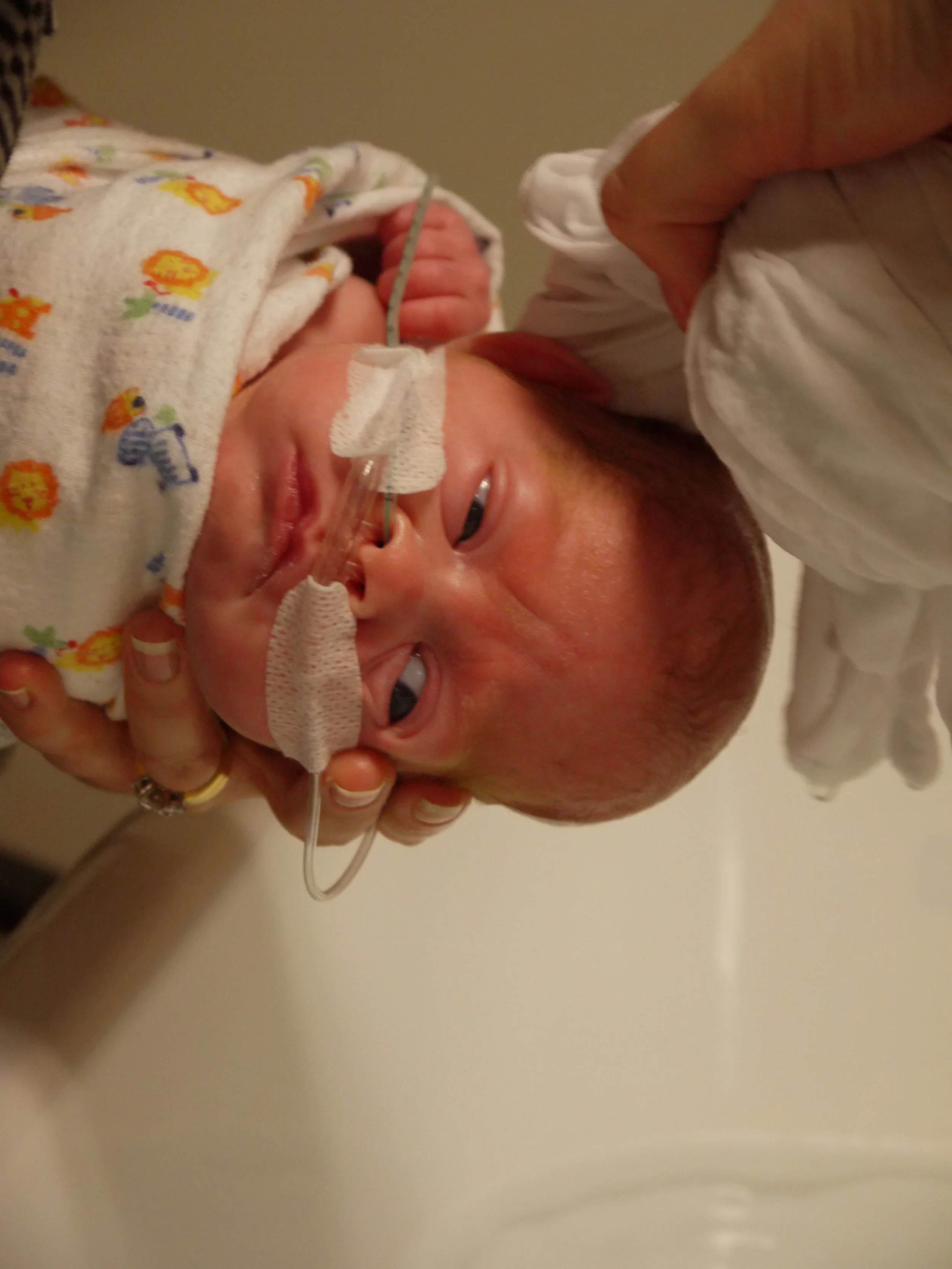
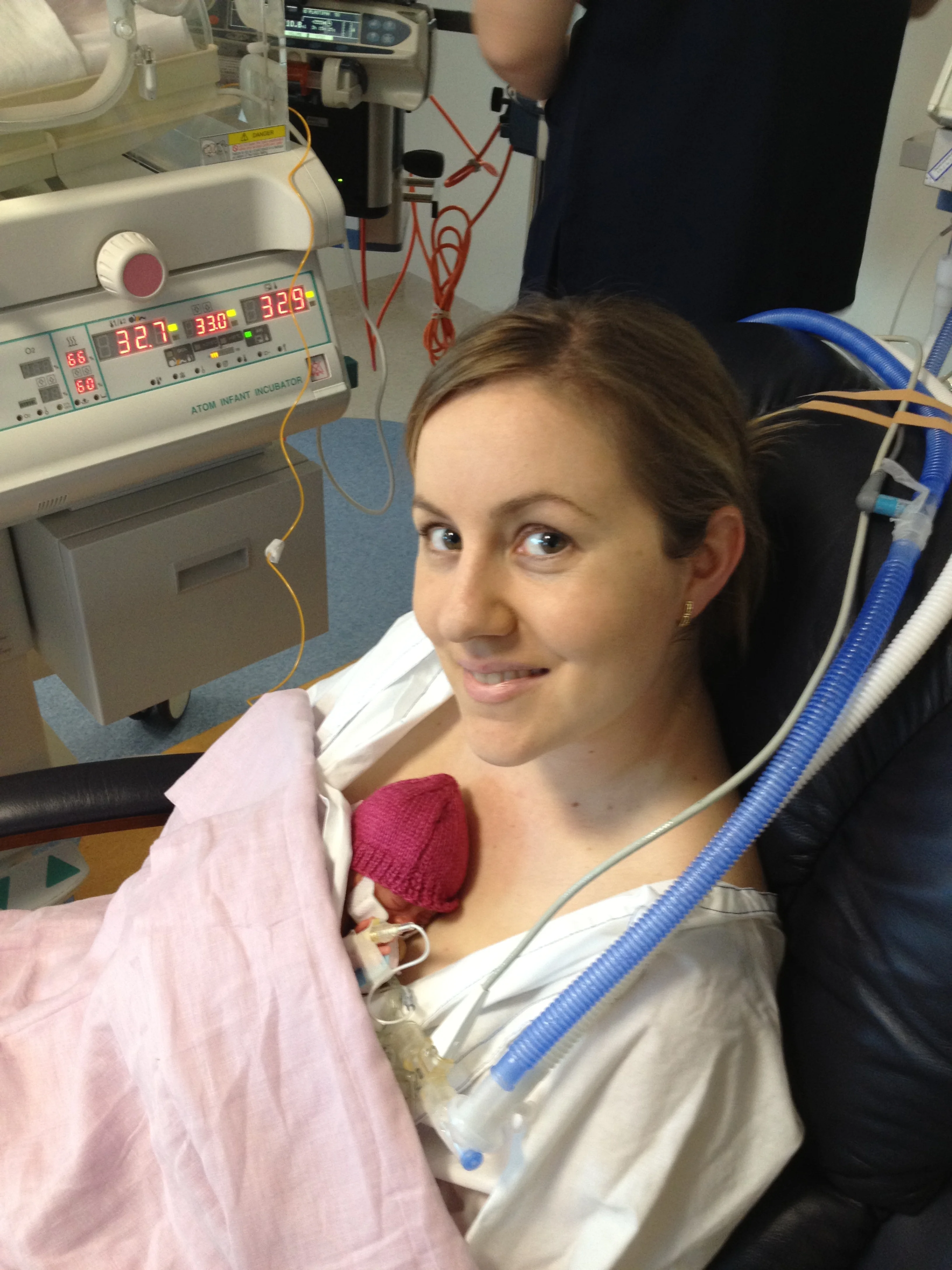
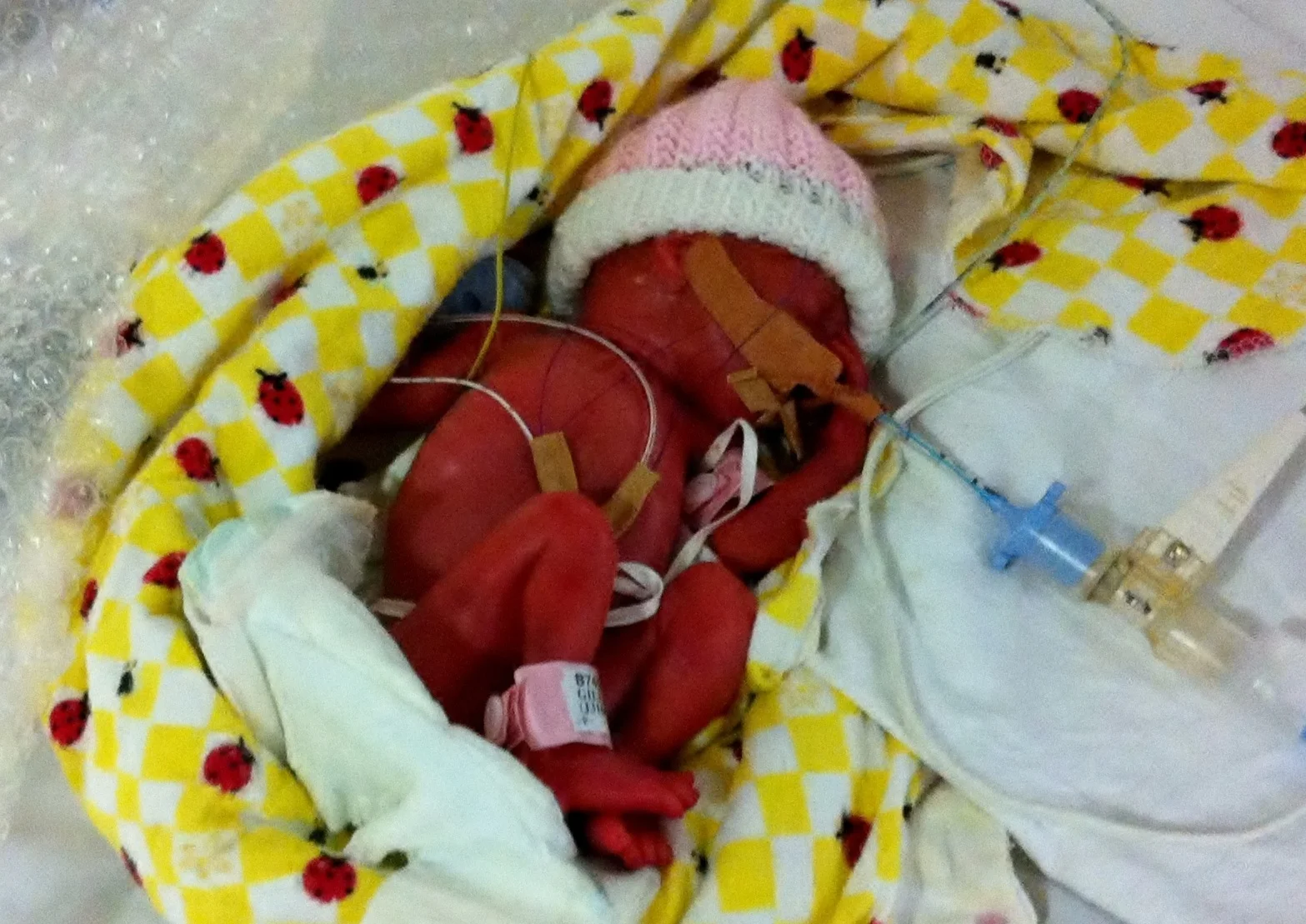
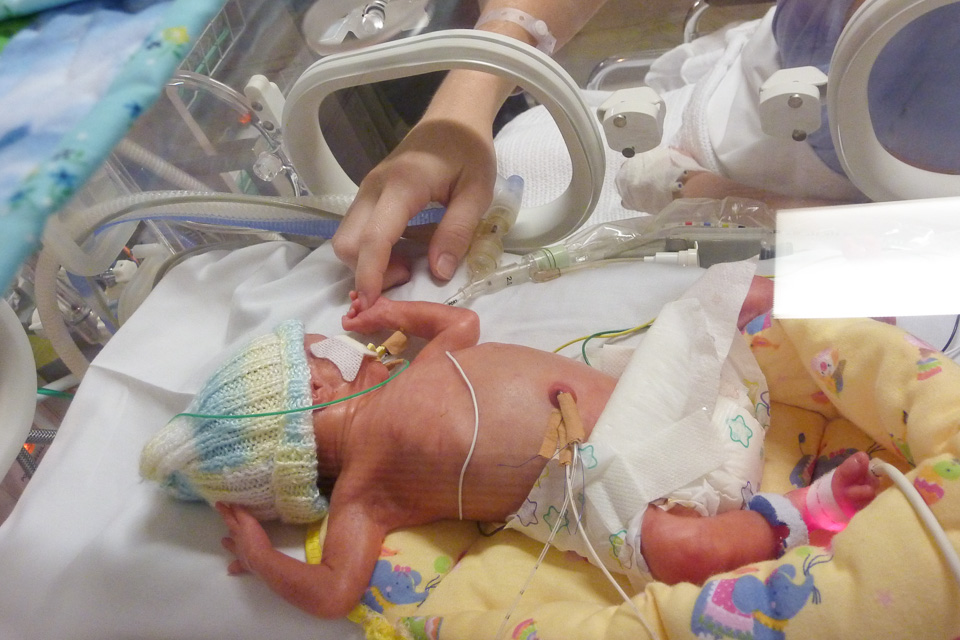
Now on CPAP and IV free, Olivia’s journey from weeks four through to her eventual homecoming are a much different story to write than that of her birth and first three weeks in NICU, although still an emotional and difficult one (see Parts I and II here).
Dan (my husband) returned to work after those first three weeks and so we started a new routine for visiting the NICU. Dan would go in either before or after work at least every second day and all day on weekends, I started driving myself in Monday to Friday. We would visit together on the weekends.
Olivia had a new neighbour during week two (we were in a pod of only 2 beds and had been by ourselves for a little while) and in the following weeks I had started talking to the baby’s mother, who would become the best company anyone could ask for in the situation, and it helped immensely when Dan had to return to work. The new baby’s mother had a previous premature baby and was a wealth of knowledge for me on expressing, routine, and what we could eventually expect when we were discharged. I will forever be grateful that our babies ended up as neighbours and that I made this new friend.
Over the next few weeks Olivia’s care and management consisted mostly of winding down her oxygen and CPAP requirements (from higher settings to lower settings) and trying to have her gain a good amount of weight. Calories were added to my expressed breast milk and on day 33 Olivia finally reached the magical 1kg mark! I had called in the early hours of the morning to check whilst awake expressing (as they weigh the babies overnight) and was so delighted to discover she had weighed in at 1000g exactly, they checked it twice! I bought in a home made caramel slice for the staff and bought a little stuffed giraffe from the gift shop for Olivia. I made a ribbon collar for it with a tag saying it was for reaching 1kg, and the giraffe is one of the many special keepsakes Olivia will have for her lifetime.
At four weeks and six weeks Olivia had blood transfusions numbers two and three (of four that she would have in total). A few days after her transfusion at six weeks Olivia’s CPAP could be turned down to its lowest setting and on day 49, at 32 weeks 3 days corrected, Olivia was able to try cycling from CPAP to PBF (oxygen via nasal prongs) for just one hour to start with. It turned out to be a big week for Olivia, on day 52 her feeds were moved from 2 hourly to 3 hourly and we also discovered that she was carrying a strand of e-coli that was mostly antibiotic resistant, picked up from another baby in the nursery. This did not make her sick, but did have the potential to, and contact precautions and restrictions on her movements through the nurseries were enacted. We were not allowed to progress normally through the nursery (to HDU and ‘Two-west’ etc) due to the contact precautions required.
Day 55 saw Olivia transferred from her humidicrib to an open cot for the first time and day 56 saw Olivia have her two-month vaccinations whilst still in NICU! I came in to the nursery at 4:30am to make sure I was there to hold her hand whilst she had the injections, I felt it was one thing that the NICU experience was not going to take away from me as a new mum, my rite of passage in holding my two month old baby whilst they got their first needles.
That weekend we received a phone call to say that Olivia would be in nursery two when we came in to see her next, they had to conduct a rearrangement of the babies carrying the e-coli bug and had set up a new quarantine area in nursery two. We were very excited at first as it felt like a ‘graduation’ of sorts, however my excitement soon turned to a couple of emotion filled days as the change impacted me more than I realized it would, or that anyone warned that it might. After 58 days of becoming used to one spot in the nursery and knowing every nook and cranny of that spot, the view out the window and the timing of the doctor’s rounds, this was suddenly rearranged and it hit me quite hard. In hindsight it is easy to describe why it was such a change, but at the time it was much harder to reconcile my emotions about the move and a tough couple of days ensued. Fortunately, Olivia’s neighbour and the baby’s mother moved with us, and her friendly company once again helped me. The feeling was mutual and she told me one day that the company and conversation was so helpful to her; we’re still in contact two and a half years later.
Although the physical move to nursery two came on day 58, Olivia became a nursery two level baby on day 71 (at 35+4 weeks corrected), when she was removed from her CPAP full time (remaining on PBF full time), had her caffeine medication ceased and her cardiac monitoring removed. This milestone also coincided with us being able to give Olivia her first proper bath at 10 weeks old!
Olivia looking a little unsure about her first bath
One of the most difficult things about the last part of any NICU baby’s journey, as any parent will attest to, is that there is no way of telling how long it will be until the end. Also, the fact they become, act and look healthier and closer to ‘normal’ newborns means that you can’t help but consider tucking them under your arm and insisting that you can handle things at home! The nursing care becomes less intensive (higher baby to nurse ratio) and the process generally becomes frustrating, a lot more frustrating.
It wasn’t until day 90 that Olivia was finally oxygen free, although we were grateful this was before her due date (at 38+2 weeks corrected), it had been a frustrating journey to that point as there had been a change of consultant in that last fortnight and different parameters had appeared to be set as to what level of de-sat would require her oxygen to be reinstated (I refer to the above paragraph detailing frustration!).
The remaining hurdle Olivia needed to master after her oxygen was removed was suck feeding, and on day 98 after a few days of having three suck feeds spaced by only one tube feed, the decision was made to remove Olivia’s feeding tube and see how she would go on all suck feeds! It was a success (just!) and on day 100 we were told that Olivia had met all the discharge requirements and was ready to go home! It was a Sunday morning and believe me, I was ready for this moment. We had installed the car seat and packed a nappy bag that week, I was ready to break out! The consultant then casually said “although, Olivia is booked for an eye exam on Monday night, perhaps you should stay until after that.” (Eye exams were required to assess for ROP, a product of prematurity and prolonged oxygen requirement. Olivia had stage 1 ROP which self-resolved).
It may have seemed fairly insignificant to the consultant to ask us to stay another two days with Olivia, and with a justifiable reason for doing so, but I’m sure every parent of a premature baby knows exactly what I would have been feeling at that moment!! “Another TWO DAYS, are you serious!?” (Yes, again refer to the paragraph on frustration!). We reached a compromise, which was that we would be immediately transferred to a mother-crafting room (where I would be able to stay overnight with Olivia for the first time ever) and stay two nights there until after the eye exam.
It was a surreal experience to be left alone with Olivia after 100 days of never having once been alone with her. There were no monitors, no nurses, no noises, it was just us. Unfortunately Dan couldn’t stay with us overnight, but he did stay until late evening each day and go home just to sleep. On day 101 we celebrated both Olivia’s due date and our wedding anniversary in the mother crafting room, after a night of four hours broken sleep (which I thought was a great effort!). My heart raced every time someone knocked on the door, I was still fearful that someone was going to announce there had been a mistake and we had to return to the nursery! After such a long time it still hadn’t sunk in that we would actually be taking Olivia home. But no one did. That evening Olivia had her final eye exam in hospital and the next morning we were told we could leave!! We tucked Olivia in to her pram and paced around the room whilst we waited for her discharge medications from the hospital pharmacy. Once we had those we wheeled Olivia out of the room and down the corridor… it was the most surreal feeling in the world and I must confess to still welling up with emotion every time I think about it! For me, the homecoming day is the most special day of the whole NICU journey and the joy I feel when I hear of any baby coming home (not just Olivia) is overwhelming!
Olivia weighed 2.6kg and measured 46cm on her due date.
Dan was fortunate enough to be able to take another three weeks off work when Olivia came home and so we made ourselves comfortable and soaked up the start of our new lives at home for that time. We were both so much in love and no amount of sleep deprivation, vomit or poo explosions were going to stop us from thinking that this was the single best thing ever!
Olivia took a very slow and steady approach to weight gain and was mostly off the bottom of the weight curve for her corrected age, but was otherwise healthy and a generally happy baby. I was extremely strict with the health of visitors to the point where we simply limited the number of visitors quite heavily for the first few months. I wasn’t keen on passing Olivia around for cuddles and trips out to public places were definitely off the table. It was a hard line approach and was isolating at times; it is one primary aspect of the ‘NICU journey’ that doesn’t actually end when you leave hospital. That, and the volume of specialist appointments that need to be attended!
However I do not regret being so strict as Olivia’s health thrived and she has not had one hospitalisation since her discharge. Two and a half years later, Olivia is still petite but otherwise a picture of health and developing on-track for her corrected age. She has just finished Level 1 ‘Surf Babies’, loves drawing, playing in sand and Peppa Pig! She is a strong willed and determined girl, no doubt a product of the battle she fought so very early in her life!
Above (L to R): Olivia in her pram on discharge day; Leaving the mother-crafting room; Olivia now.
You may also like these stories: