This is part 3 of a 4 part series. You can read part 1 here and part 2 here.
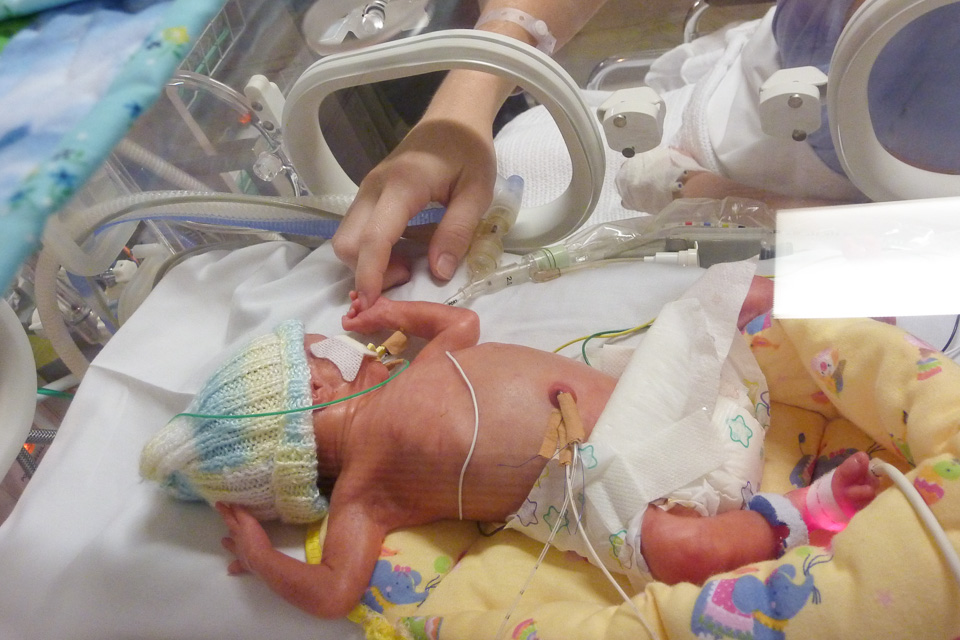
Bringing Adison home to our family was amazing. His entire NICU stay he was unable to meet his siblings as the NICU has a strict parents only visitation policy. The children were overjoyed at meeting their new brother but also cautious knowing just how fragile he was and how close he'd come to never coming home at all.
Around 6 weeks after coming home i became concerned for Adison's health. He was lethargic, not nursing well, irritable and having grey spells when travelling in the car. Both the local ER and his followup NICU paediatrician brushed off my concerns but i knew something wasn't right. At our routine cardiology appointment it was revealed that Adison was in the preliminary stages of heart failure. He had left the NICU with a patent ductus arteriosis (PDA) which had now caused pulmonary hypertension, meaning that the blood rushing to his lungs was at too high pressures thus putting his heart under extra pressure.
The cardiologist was confident that the pressures could be controlled with medication so that was organised and we were sent on our way. The plan was for a catheter procedure to plug the PDA when Adison was around 1 year old or 10kg whichever came first. Just 3 days later, after 5 doses of medication we landed ourselves in the local hospital ER. Adison had rapidly deteriorated and had had an unprecedented reaction to the medication where the pressures drop too low, it was a scary time. We were immediately transferred to PMH and the Doctors kept us waiting a couple more days whilst they worked out a plan of attack and made sure PICU beds were available.
Post op in PICU. I had a mild irrational panic when i saw him, my baby, on a big bed, with no side rails. He was heavily sedated and not going anywhere!
Yet again we were at life and death cross roads. I was taken to the surgeons office to consent to a thoracotomy and PDA ligation. They would make an incision on Adison's back under his shoulder blade, enter between the ribs and manually tie off the offending artery which runs between the heart and lungs. The surgeon made it clear that without the surgery Adison's heart would ultimately fail and he would pass away. With the surgery there was a very real risk that the main artery to the heart may tear as they went to tie off the PDA which would cause him to bleed out on the table. I had to trust in the steady hands of the surgeon and the strength of my son and sign the consent. There was no other real option. Russell and our other children were home in Australind and again I was faced with this confronting situation alone.
Whilst 6 months had passed since Adison's birth he was still a tiny 4.5kg. Hours past and finally I was told that everything was successful and Adison would be spending quite some time in PICU ventilated and sedated until they were sure that everything would be ok. 10 days later we were discharged. Adison was doing much better but this had been a significant setback that would take him many months to overcome. Adison came home on a hospital apnoea monitor and nocturnal oxygen. Damage had been caused to his lungs and he required additional support whilst sleeping. He was also having regular apnoeas and no one was quite sure why. Sleep studies later revealed the apnoeas were caused by his premature central nervous system.
Home oxygen.
I can sit! 1 year old and still tiny in size 000 clothes.
3 years on and we have had numerous admissions to hospital for pneumonia requiring oxygen for many days, sleep studies, MRI, 2 sets of grommets and his adenoids removed.
Adison's gross motor skills were very delayed, he rolled at 9m, sat at 13m, and didn't walk until 22m. He was on home oxygen until he was 18m at which time he could finally maintain stable levels of oxygen whilst sleeping. Adison continues to suffer from chronic lung disease and is very susceptible to cold and flu bugs. The challenges don't stop there, we attend speech, occupational therapy, physiotherapy and numerous specialist follow up appointments to help Adison become the best person that he can be.
In spite of the labels that follow Adison around the medical world, chronic lung disease, cerebral palsy, hypotonia, verbal & oral dyspraxia, dysarthria, sensory processing disorder, he is an amazing, bright, confident little boy who's catching up, every moment of every day.
Look at me now! Just one of the gang.
You may also like these stories :